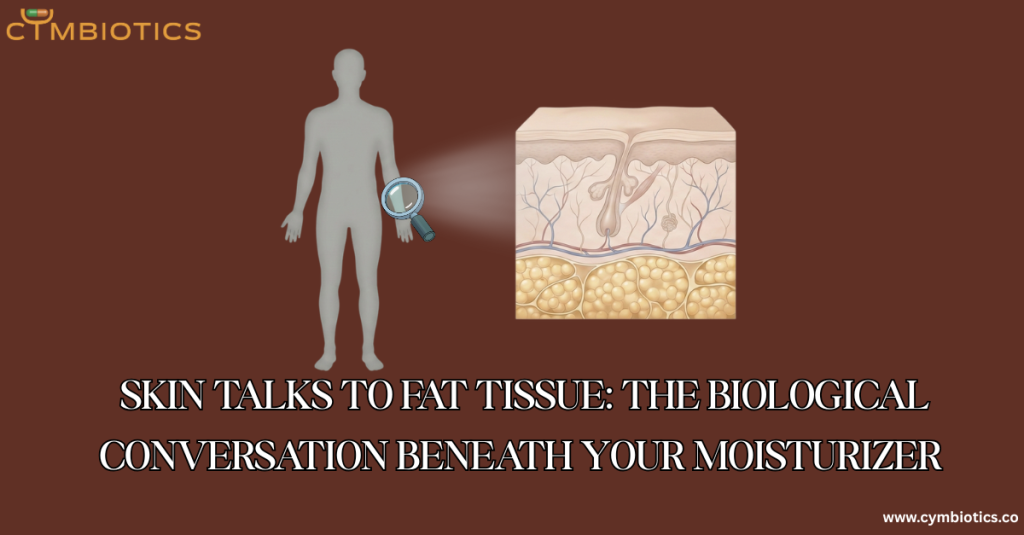
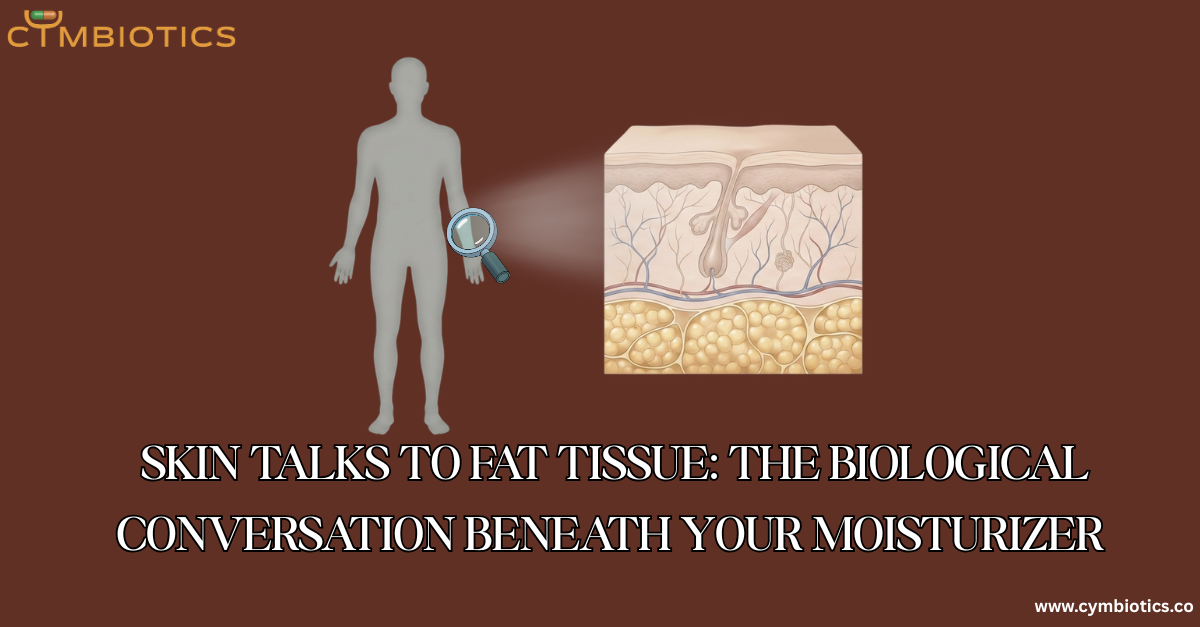
When we think about skin health, we usually stop at the surface.
Barrier. Hydration. Collagen. Microbiome.
But beneath the dermis lies an active, metabolically dynamic layer that rarely gets attention in skincare conversations: subcutaneous adipose tissue.
Fat is not passive storage.
It is a signaling organ.
And your skin is constantly listening.
Beyond Storage: Adipose Tissue as an Endocrine Organ
For decades, adipose tissue was considered inert, a reservoir for energy.
We now know it functions as an endocrine organ, producing signaling molecules called adipokines. These include:
- Leptin
- Adiponectin
- Resistin
- Pro-inflammatory cytokines (e.g., TNF-α, IL-6)
These mediators influence systemic metabolism, immune regulation, vascular tone and importantly, skin biology.
Subcutaneous fat and dermal tissue are not isolated compartments. They communicate through soluble factors, immune cell trafficking, and vascular networks.
The Dermal White Adipose Tissue (dWAT) Layer
Emerging research identifies a specialized layer known as dermal white adipose tissue (dWAT).
This layer:
- Participates in wound healing
- Modulates inflammatory responses
- Contributes to hair follicle cycling
- Influences fibrosis and scarring
Adipocytes within dWAT can even transform into myofibroblast-like cells during injury repair, demonstrating functional plasticity.
This means fat is actively involved in tissue remodeling, not just cushioning.
Adipokines and Skin Inflammation
Adipokines can either promote or regulate inflammation.
For example:
- Leptin promotes pro-inflammatory signaling and may enhance keratinocyte proliferation.
- Adiponectin has anti-inflammatory and barrier-supportive effects.
- Elevated IL-6 and TNF-α from adipose tissue can influence dermal immune activity.
In conditions of metabolic imbalance or chronic stress, adipose tissue shifts toward a pro-inflammatory phenotype.
That shift doesn’t stay localized.
It influences skin tone, reactivity, repair speed, and even aging trajectories.
Skin Aging and Adipose Signaling
Facial aging isn’t just collagen loss.
Changes in subcutaneous fat distribution alter:
- Mechanical support
- Vascular supply
- Paracrine signaling
Reduced adiponectin levels have been associated with increased oxidative stress and inflammatory tone, both contributors to cutaneous aging.
Meanwhile, chronic low-grade inflammation from adipose tissue can accelerate matrix degradation.
Aging, therefore, is partly a conversation between fat and fibroblasts.
Wound Healing: A Collaborative Effort
During injury:
- Adipocytes release inflammatory mediators.
- Immune cells are recruited.
- Fibroblasts are activated.
- Angiogenesis increases.
Dermal adipocytes can rapidly expand and contract in response to injury signals.
This dynamic response supports early defense and later remodeling.
Without proper adipose-dermal communication, wound healing is delayed or dysregulated.
The Energy–Inflammation Axis
Adipose tissue sits at the intersection of:
- Metabolism
- Immune signaling
- Structural integrity
Energy surplus, sleep deprivation, chronic stress, and metabolic imbalance alter adipokine secretion patterns.
Skin reflects these shifts.
Inflammation rises. Repair efficiency falls. Barrier recovery slows.
The biological conversation beneath your moisturizer becomes noisier.
Why This Matters for Skincare
Most topical formulations focus on:
- Surface hydration
- Barrier lipids
- Epidermal turnover
Few acknowledge that dermal and subcutaneous signaling environments shape how skin behaves.
You cannot separate structure from metabolism.
Supporting skin resilience requires respecting the interconnected system beneath it, including vascular health, metabolic balance, and inflammatory tone.
The Cymbiotics Perspective
At Cymbiotics, we view skin not as a layered surface problem, but as a multilayer biological ecosystem.
Barrier support matters. But so does:
- Inflammatory modulation
- Cellular energy dynamics
- Microvascular integrity
- Signaling balance
Healthy skin is not just well-moisturized.
It is well-regulated.
Understanding adipose–dermal communication reframes skincare from surface correction to biological stewardship.
Because beneath every moisturizer lies a living conversation.
References
- “Dermal white adipose tissue: Development and impact on skin defense and fibrosis” – Peng Y., Cheong S., Lu F., He Y. FASEB Journal, 2024.
- “Dermal white adipose tissue: A newly recognized layer of skin innate defense” – Chen S.X., Zhang L.J., Gallo R.L. Journal of Investigative Dermatology, 2019.
- “Adipokines in the skin and in dermatological diseases” – Kovács D., Fazekas F., Oláh A., Törőcsik D. International Journal of Molecular Sciences, 2020.
- “Adiponectin regulates cutaneous wound healing by promoting keratinocyte proliferation and migration via the ERK signaling pathway” – Shibata S., Tada Y., Asano Y., et al. Journal of Immunology, 2012.
- “Dermal white adipose tissue: A new modulator in wound healing and regeneration” – Wu Z., Wang Z., Chen T., et al. Regenerative Therapy, 2024.
- “Subcutaneous adipose tissue: Implications in dermatological diseases and beyond” – Ziadlou R., Pandian G.N., Hafner J., et al. Allergy, 2024.